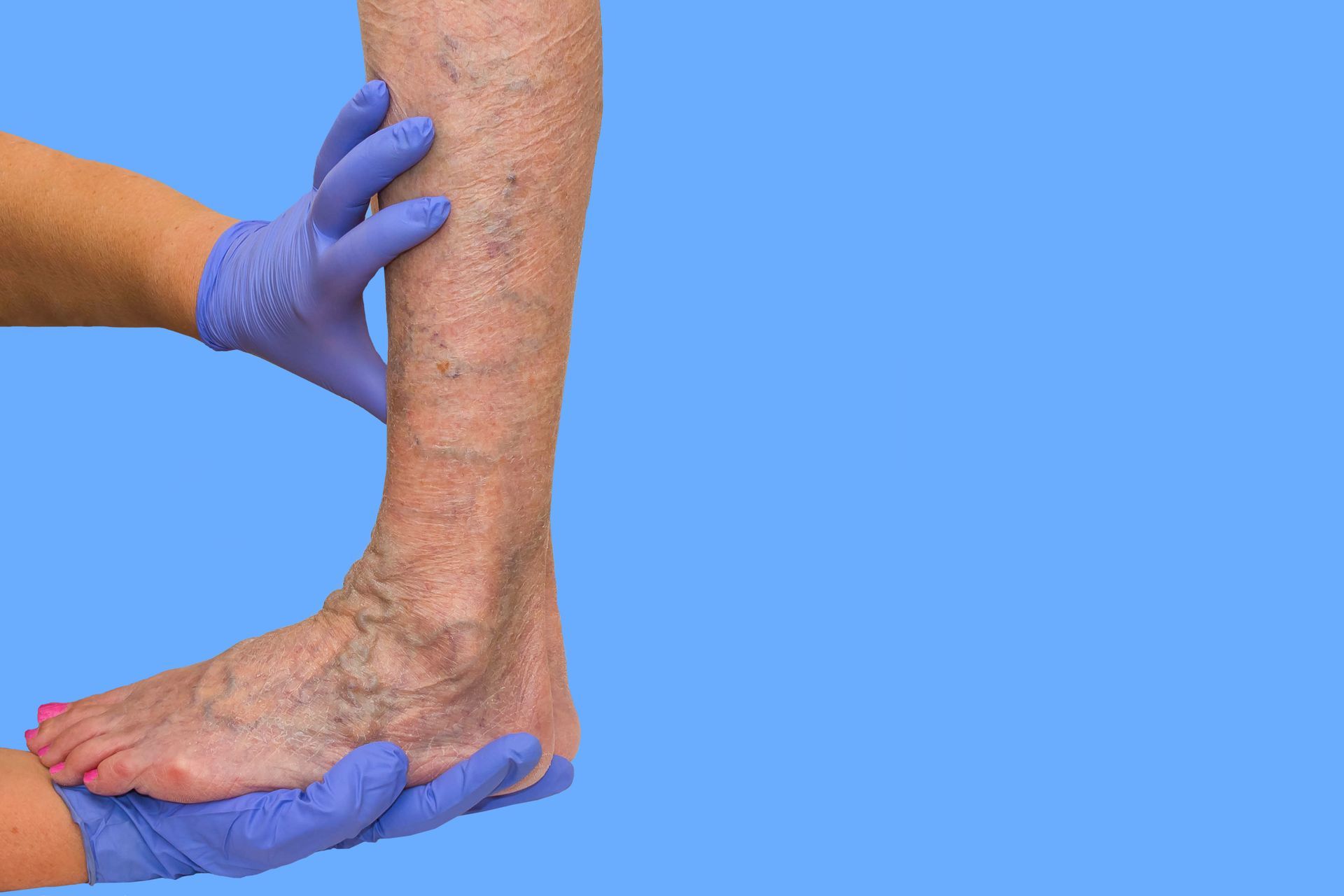
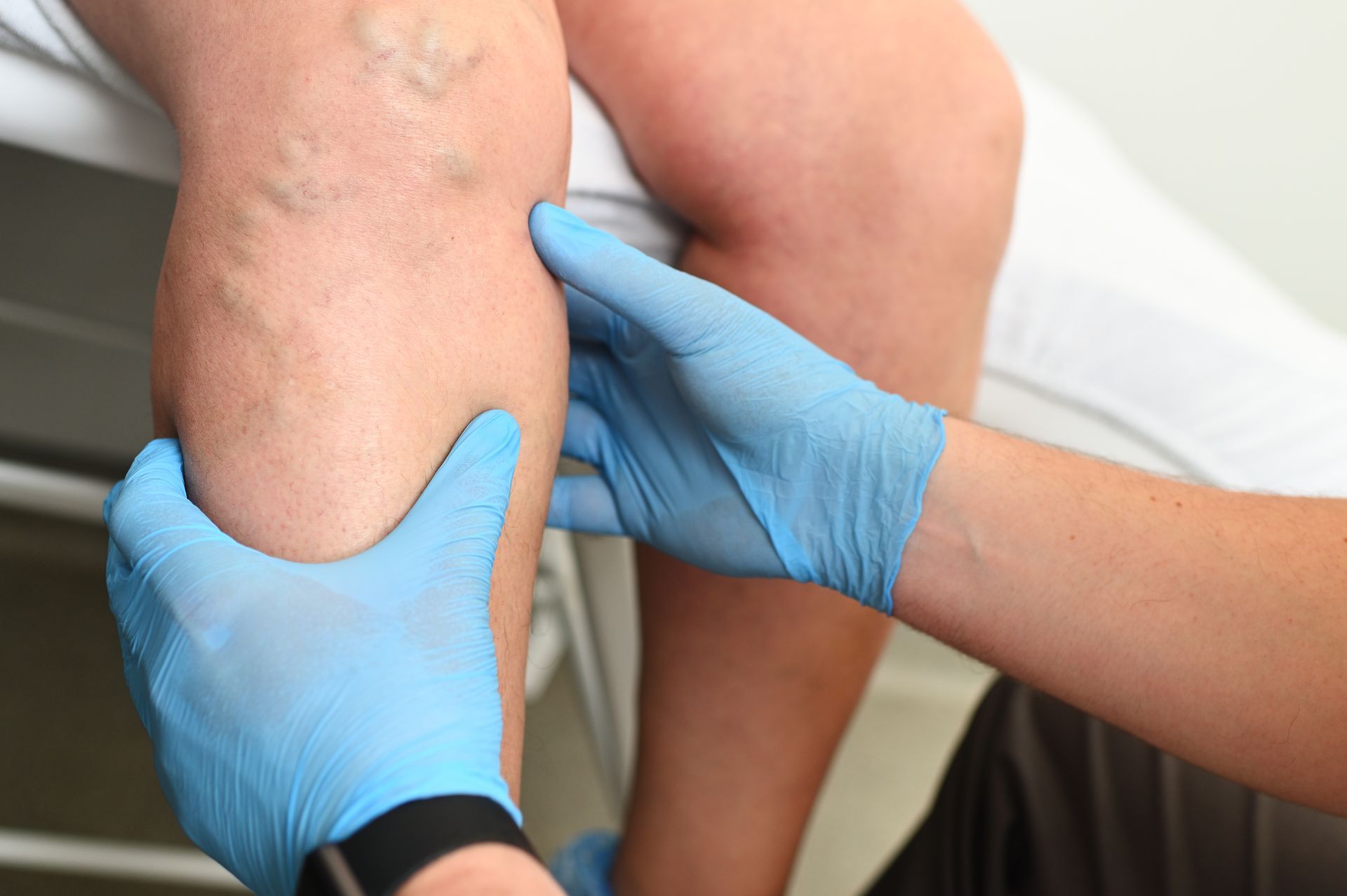
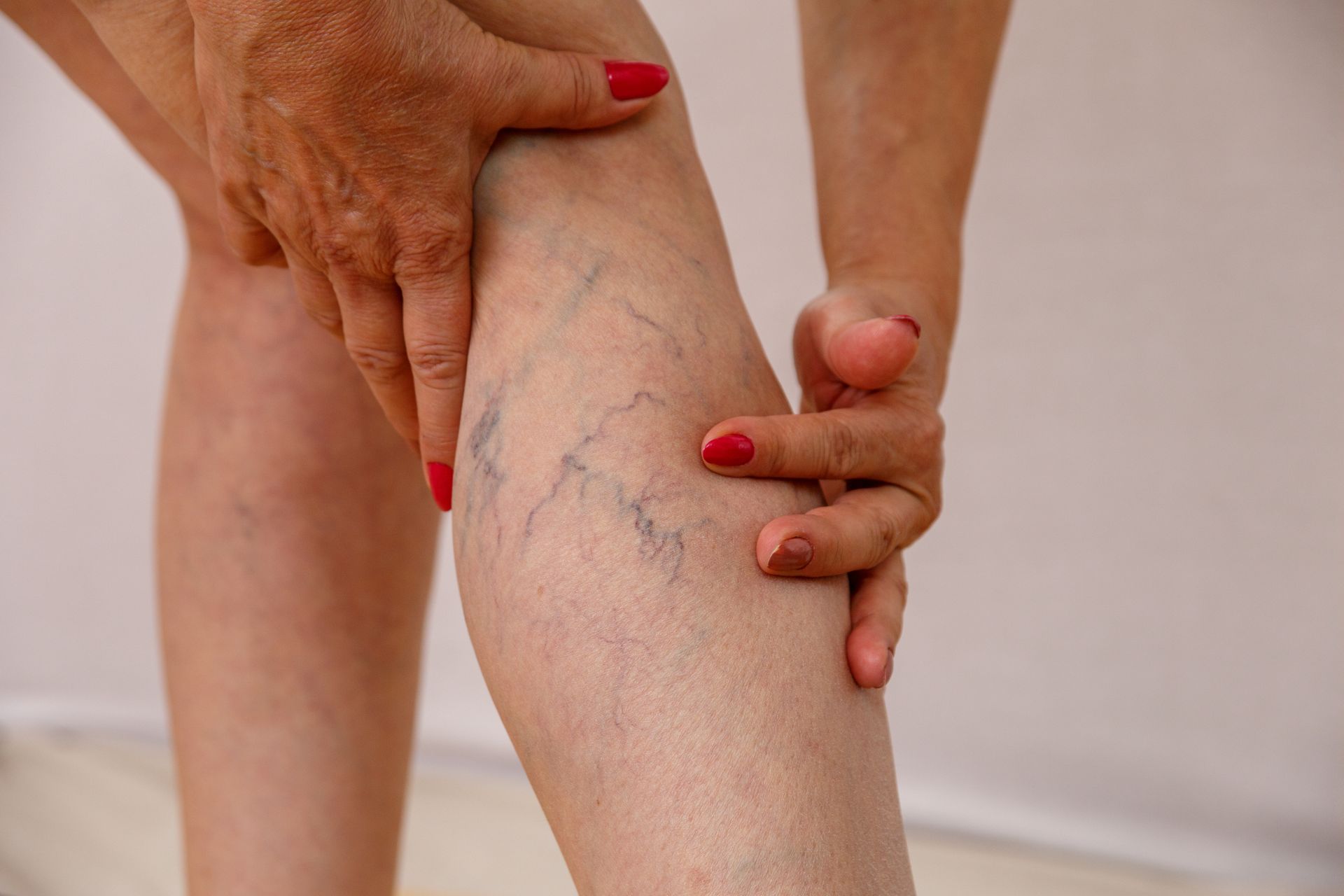
Understanding Chronic Venous Insufficiency (CVI) and How It’s Treated
If your legs often feel heavy, swollen, or tired by the end of the day, it may be more than simple fatigue. These symptoms are commonly associated with Chronic Venous Insufficiency (CVI)—a progressive vascular condition that affects blood flow in the legs and, if left untreated, can lead to more serious complications.
At California Vascular Health Specialists, early recognition and expert care play a critical role in preventing CVI from advancing and helping patients return to a more comfortable, active life.
What Is Chronic Venous Insufficiency?
Chronic Venous Insufficiency occurs when the veins in your legs struggle to send blood back up to your heart. Healthy veins rely on tiny one-way valves to keep blood moving in the right direction. When those valves weaken or become damaged, blood can begin to flow backward and pool in the lower legs.
Over time, this added pressure inside the veins leads to inflammation, visible vein changes, and worsening symptoms. While CVI develops gradually, it does not resolve on its own—making early intervention essential.
What Causes CVI?
CVI is most often caused by venous valve dysfunction, but several underlying conditions and lifestyle factors can contribute to its development.
One of the most common causes is a history of blood clots, also known as deep vein thrombosis (DVT), which can damage the valves. Other contributing factors include naturally weakened vein walls, aging, and genetic predisposition.
Certain lifestyle and health factors can increase your risk, including:
- Standing or sitting for long periods
- Obesity
- Pregnancy
- Smoking
- Family history of vein disease
Because these risk factors are common, many people may be living with early-stage CVI without realizing it.
Signs and Symptoms to Watch For
CVI symptoms often start subtly and worsen over time. Many patients initially dismiss them as normal fatigue or aging. However, recognizing these early warning signs can make a significant difference in treatment outcomes.
Common symptoms include:
- Swelling in the lower legs or ankles
- A feeling of heaviness or aching
- Visible varicose or spider veins
- Skin discoloration or darkening
- Itchy or irritated skin
- Nighttime leg cramps
As the condition progresses, symptoms can become more severe. In advanced cases, patients may develop venous ulcers—slow-healing wounds typically near the ankles that require specialized care.
Why Early Treatment Matters
Chronic Venous Insufficiency is not just a cosmetic issue—it’s a medical condition that tends to worsen over time.
Without proper treatment, CVI can lead to:
- Persistent pain and swelling
- Skin damage and inflammation
- Increased risk of infection
- Open sores or ulcers
The earlier CVI is identified, the more treatment options are available—and the easier it is to prevent long-term complications.
How CVI Is Diagnosed
Diagnosing CVI is straightforward and non-invasive. A vascular specialist will begin with a physical examination and a discussion of your symptoms and medical history.
The most important diagnostic tool is a duplex ultrasound, which allows providers to evaluate blood flow in real time and identify any valve dysfunction or venous reflux. This imaging is painless and plays a key role in developing a precise, personalized treatment plan.
Treatment Options for Chronic Venous Insufficiency
The goal of CVI treatment is to improve circulation, relieve symptoms, and stop the condition from progressing. Fortunately, modern vascular care offers a range of effective solutions.
Conservative Treatment
In early stages, simple lifestyle adjustments can significantly improve symptoms:
- Wearing medical-grade compression stockings
- Elevating the legs throughout the day
- Staying active to promote circulation
- Managing weight
- Avoiding prolonged sitting or standing
These strategies help reduce pressure in the veins and support healthier blood flow.
Minimally Invasive Procedures
For patients with more advanced symptoms, minimally invasive treatments can provide lasting relief. These outpatient procedures are highly effective and require little to no downtime.
Common options include:
- Endovenous laser therapy (EVLT)
- Radiofrequency ablation (RFA)
- Sclerotherapy
These treatments work by closing or redirecting blood flow away from damaged veins, allowing healthier veins to take over. Patients often notice a significant reduction in symptoms and visible veins after treatment.
Living With CVI
Although CVI is a chronic condition, it is highly manageable with the right care. Patients who follow a personalized treatment plan often experience:
- Reduced swelling and discomfort
- Improved mobility
- Healthier skin
- Better overall quality of life
Consistency is key. Ongoing care, lifestyle habits, and routine follow-up visits help maintain long-term results.
When Should You See a Specialist?
It’s time to seek a vascular evaluation if you notice:
- Ongoing leg swelling or heaviness
- Prominent varicose veins
- Skin discoloration near the ankles
- Pain that worsens throughout the day
- Wounds that are slow to heal
These symptoms may indicate underlying venous disease that should be addressed before it progresses further.
Expert Vein Care You Can Trust
At California Vascular Health Specialists, patients receive comprehensive, individualized care backed by advanced diagnostic tools and modern treatment options. The focus is always on identifying the root cause of symptoms and delivering solutions that provide real, lasting relief.
If you’re experiencing signs of Chronic Venous Insufficiency, seeking care early can make all the difference—not just in how your legs feel, but in your long-term vascular health.